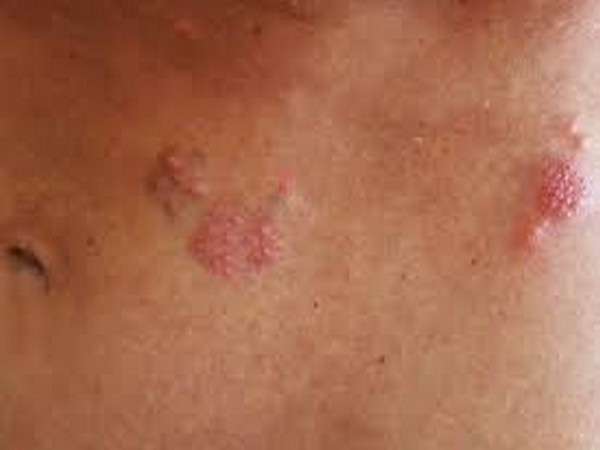
Washington: A recent study has observed that the chickenpox vaccine not only protects against chickenpox but it also decreases the risk for shingles (a painful skin rash with blisters).
Shingles, or herpes zoster, is caused by the varicella-zoster virus, the same virus that causes chickenpox. However, pediatric HZ (herpes zoster) is a rare disease, and the symptoms are usually milder for children compared with adults, who typically report a painful, burning, and blistering skin rash.
“Since the introduction of the chickenpox vaccine, we have known how effective it is in preventing children from contracting that itchy and painful disease, but we set out to determine if the vaccine would also reduce risk of herpes zoster. Our findings demonstrate that the vaccine does reduce the likelihood of shingles in kids, highlighting the dual benefits of the chickenpox vaccine,” explained lead investigator Sheila Weinmann in the Journal of Pediatrics.
The study looked at the electronic health records of more than 6.3 million children between 2003 and 2014, using data from 6 integrated health care organizations. Approximately 50 per cent of the children were vaccinated for some or all of the study period.
Researchers found that, overall, HZ risk is much lower in vaccinated than unvaccinated children. Specifically, they concluded that, over the 12-year period of the study, the rate of pediatric HZ declined by 72 per cent overall as the number of vaccinated children rose.
Secondly, incidence of HZ was 78 per cent lower in vaccinated children than in unvaccinated children and rates for immune suppressed children, who were unable to receive the vaccination, were five to six times higher than for those who were not immune suppressed.
“We looked at the incidence rates of HZ overall, at how many cases there were per 100,000 person-years, including by age and gender.
Person-years refers to the type of measurement that takes into account both the number of children who were included in the HZ study and the amount of time each child spent in the study over its 12-year course. We saw the highest rates of HZ in the early years of the study when there were a higher proportion of children, particularly older children, who had not received the varicella vaccine,” noted Weinmann.
The rate of HZ among children who were unvaccinated climbed from 2003 to 2007 and then declined sharply through the end of the study period. Increasing rates of vaccination over the study period reduced the risk of contracting HZ overall for all children, including those who were unvaccinated. The decline could also have been related to the introduction of the second vaccine dose beginning in 2007, as HZ incidence was much lower in those children who received the 2-dose vaccinations rather than 1-dose vaccination.
[source_without_link]ANI[/source_without_link]