Hyderabad: There is a lot of fear and panic in the general population regarding the COVID 19 infection due to the significant fatalities associated with it. The pandemic grew from an outbreak affecting thousands in Wuhan, China, to some 14.5 million cases and 600,000 deaths globally as of mid-July. “Even though death from this infection has been relatively low in India around 2.3 per cent, given the very large number of people infected, the numbers are significant,” said Dr. Narendranadh Meda (MS (Gen. Surgery), DNB (Vascular Surgery), Fellowship in Vascular Surgery (USA), and Chief Consultant Vascular & Endovascular Surgeon Foot Care Specialist, KIMS Hospitals).
Based on early reports, the COVID-19 was thought to be a standard variety respiratory virus with no vaccine and no treatment. Since then, we have also learned that corona attacks not only the lungs, but also various parts of body, like the kidneys, heart, intestines, liver and brain.
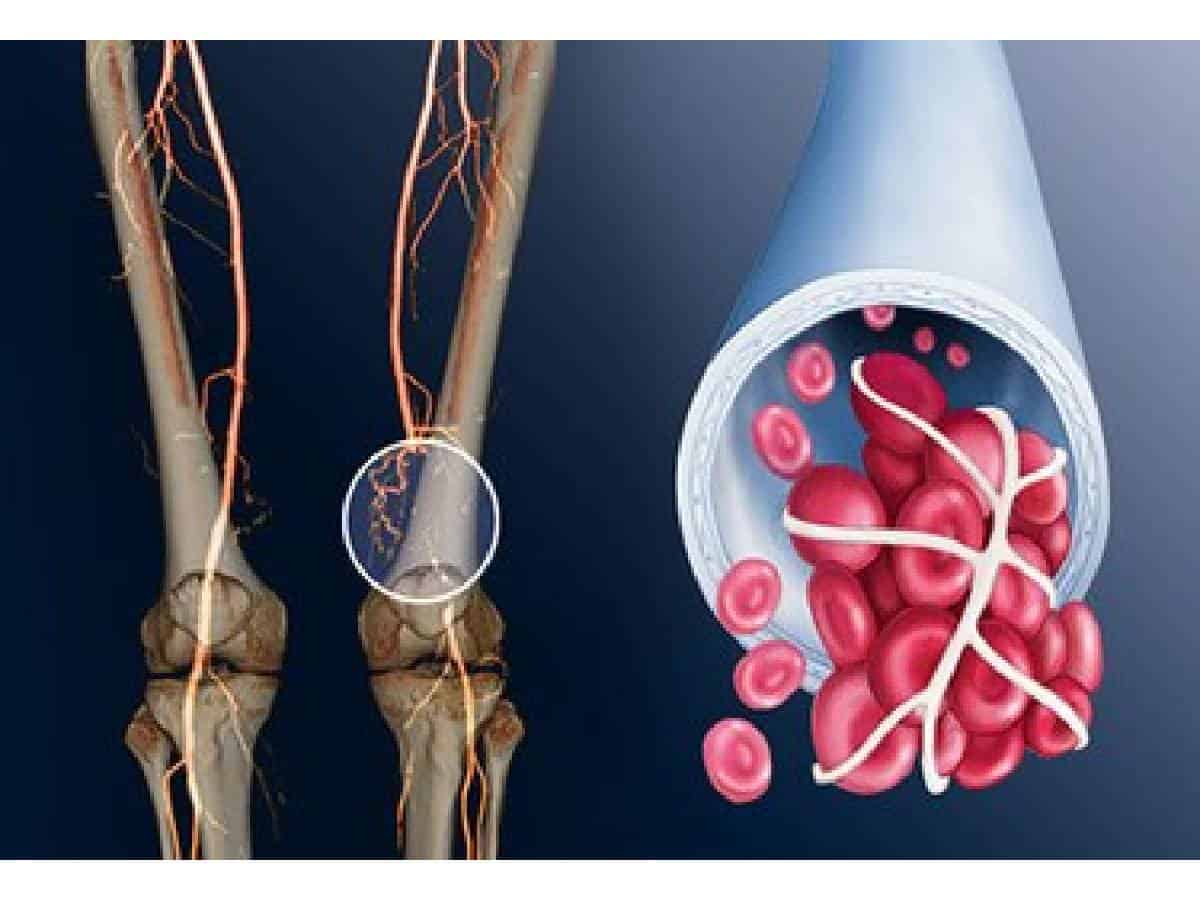
In our hospital over a period of one month, we have seen about 25-30 per cent of patients presenting with some or the other form of blood clots, either in brain presenting as stroke or in veins presenting as DVT and in arteries presenting as acute limb ischemia. In the last one month, we operated 14 COVID positive cases with clots in leg arteries (ACUTE LIMB ISCHEMIA) on an emergency basis whose presenting symptom was leg pain, said Dr Narendranadh Meda. Around six patients lost their limb due to delay in presentation. Even three cases of severe clots in the veins (Deep Vein Thrombosis) were observed with the pulmonary embolism while causing severe compartment syndrome, leading to mortality.
Very early reports suggest patients with COVID-19 infection presenting to hospitals had elevated levels of d-dimer, a marker of thrombosis in the blood vessels.
According to a study published in the Journal of American College of surgeons in May 2020, they observed COVID-19 causes not only hypercoagulability, but also fibrinolysis (ability to breakdown clots) shutdown, which is associated with blood clots in legs, stroke, and renal failure. They observed that despite thromboprophylaxis of patients, venous thrombosis developed, with pulmonary embolism (PE) being the most common. Instances of arterial thrombosis including ischemic strokes, leg clots leading to loss of limbs were also noted.
China identified one of the receptors by which the coronavirus, SARS-CoV-2, enters cells. It was the same gateway, called the ACE2 receptor, that the original SARS virus used. Studies going back some two decades had mapped the body’s ACE2 receptors, showing that they’re in cells that line the insides of blood vessels in what is called vascular endothelial cells, in cells of the kidney’s tubules, in the gastrointestinal tract, nasal epithelium and even in the testes.
A small examination of critically ill COVID-19 patients according to a study lead by Dr. Herman Poor at Mount Sinai Hospital in New York City found patients with the most severe COVID related pneumonia and respiratory distress showed immediate improvements when they were given drugs that break up blood clots.
Corona predisposes patients to a prothrombotic state (prone to clot formation) with demonstrated microvascular involvement. The degree of hypercoagulability appears to correlate with the clinical outcome.
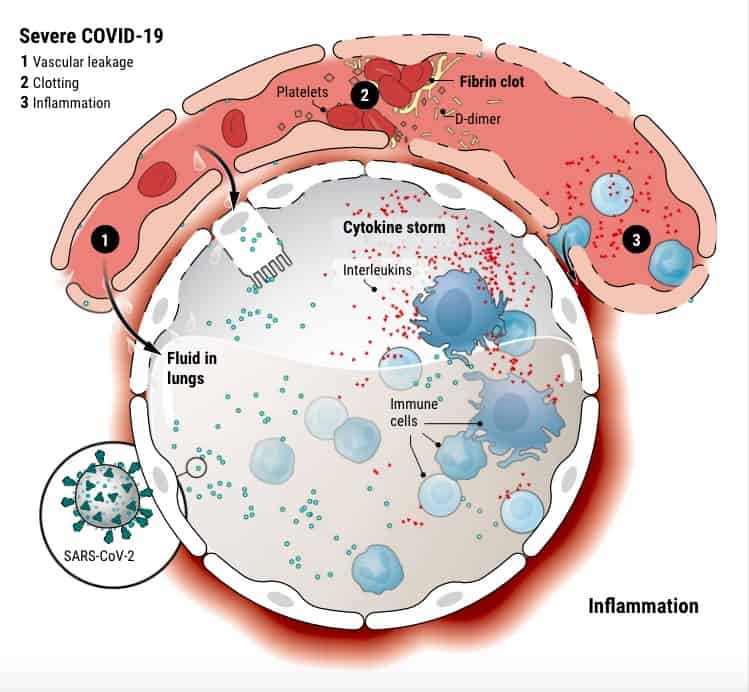
Unlike what we see in regular viral infections affecting the lung, COVID is thought to be causing early and progressive clotting of blood in the lungs (pulmonary thrombosis), which impairs blood, supply and gas exchange leading to respiratory failure. Thromboembolic disease (blood clots) is now recognized as a “frequent and concerning complication” among patients hospitalized with COVID-19.
The critical need, therefore, is for early recognition and intervention with blood thinners (anti-coagulation) in this illness and with appropriate doses.
This can be easily implemented in all hospitals based on some simple assessments:
The rate of breathing at rest (say above ~20/minute) and lowered level of oxygen in the finger (pulse-oximeter, which is easily checked in hospitals at presentation – less than 93%) even when they look relatively well.
If possible, d-dimer levels should be checked immediately. If found to be elevated (more than two-three folds above normal), this would indicate the evolving condition in the lung. Such patients should immediately receive commonly used blood thinners such as heparin or low molecular weight heparin (LMWH) in therapeutic doses until the symptoms resolve.
In those with higher risks of complications, preventive doses of LMWH have been advised soon after diagnosis. These medicines may be contraindicated in certain situations. So proper medical supervision is necessary. Careful monitoring of adverse effects must also be done.
It is important therefore that the public as well as health care professionals be aware of this problem of blood clots in these patients whose severity is unique to COVID -19. There is of course need for more studies to determine the right doses at the right stages of the disease.
This strategy has been shown to be effective and early intervention could help reduce the mortality due to COVID-19 infections in India even further.
Understanding how to prevent blood clots is important to stay healthy in everyday life, but is critical when you become ill, especially with COVID-19.
1. Not to take bed rest
2. Stay hydrated, stay active,
3. Need to do leg physiotherapy (doing regular ankle pumps) and breathing exercises.
Seek prompt medical attention if you develop leg swelling, sudden pain or difficulty breathing during your home quarantine.