New Delhi: Not all patients with Covid-19 need ventilators. For nearly one hundred days, confirmed cases of Covid-19 in India’s cities were being admitted to hospitals, irrespective of the severity of disease.
This blunder with no clinical justification crushed the entire health systems, doctors said to Indian Express. The hospitals were rendered incapable of caring for tens of thousands of other patients with non-Covid-related diseases.
There are a finite number of possibilities that can occur, when someone is exposed to Covid-19.
Asymptomatics: Of all who get exposed to Covid – 19, most will be asymptomatic: they will show no symptoms, but will continue to spread it.
Presymptomatics, mild: Of the few that are symptomatic, all will first be pre-symptomatic. This is the roughly two-day interval in which they will be contagious, will spread the virus, but will not have developed symptoms. Eventually they will develop one or a combination of the Covid-19 symptoms we recognise: loss of smell or taste, cough, fever, and so on.
Most of these symptomatic cases will only have mild symptoms not in need of any treatment, except what physicians appropriately call “symptomatic management”, with medications to simply manage the fever and cough and body aches. Home remedies may help with some of this although there is no evidence that they alter the course of the disease.
Symptomatics, moderate: Of the remainder, some will develop moderate symptoms, and some will develop severe disease. Only these two categories need sophisticated medical intervention.
Those with moderate symptoms will benefit from oxygen therapy, and “pronation,” which means lying on your belly, instead of your back. Doing so opens up the air chambers in the back of your lungs that are normally collapsed, thereby providing more oxygen to your blood.
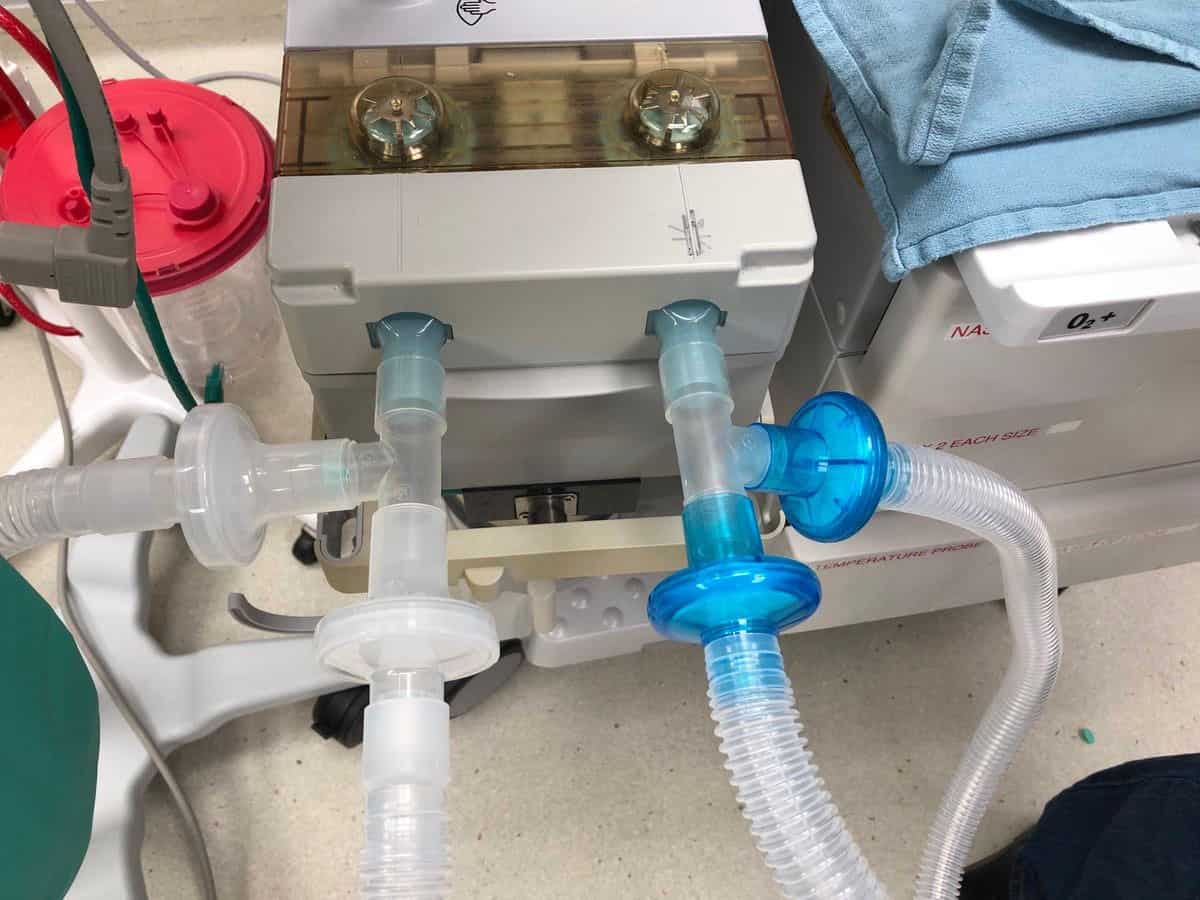
For those with moderate severity a principle intervention is oxygen — which can be delivered through a mask and tube connected to a portable oxygen tank. Many people with lung diseases have them at home. There is no clinical justification to take up ICU beds for these patients. They do not need ventilators, or intensive care specialists.
Severe cases: We have observed that the shortness of breath in patients with Covid-19 can progress abruptly, and these patients need ventilators. These breathing machines are highly complex systems that need skilled technicians to run them, and require that patients have a flexible plastic tube advanced into their trachea (windpipe), typically by an anaesthesiologist or emergency physicians or intensivists.
The patients then have to be kept sedated with a precisely dosed intravenous medication an overdose of which can easily kill the patient. And finally, plasma donated from Covid-19 survivors has also played its role.