The first case of MonkeyPox was reported in India on July 15. It was, incidentally also the first one from the entire South East Asian region as per the WHO. A 35-year-old man who arrived from the Gulf into Kerala was detected with it.
In the next 10 days three more cases (2 in Kerala and 1 in Delhi) have been detected in the country. One case of suspected MonkeyPox has been reported from Kamareddy in Telangana State, raising alarm bells.
Even as India became vigilant on the spread of this virus, the WHO Director General Tedros Adhanom Ghebreyesus declared that the rapidly spreading MonkeyPox outbreak represents a global health emergency.
At a media conference in Geneva on July 23 he said, “Although I am declaring a public health emergency of international concern, for the moment this is an outbreak that is concentrated among men who have sex with men, especially those with multiple sexual partners.”
So far this year, globally a total of 16,000 cases in more than 75 countries, including five deaths in Africa have been reported. The viral disease has been spreading chiefly in men who have sex with men in the recent outbreak, outside Africa where it is endemic.
What is MonkeyPox
The virus, which basically affects simians, was first reported in the Democratic Republic of Congo in the 1970s. It has been dormant and localised to central and west Africa in the past 50 years.
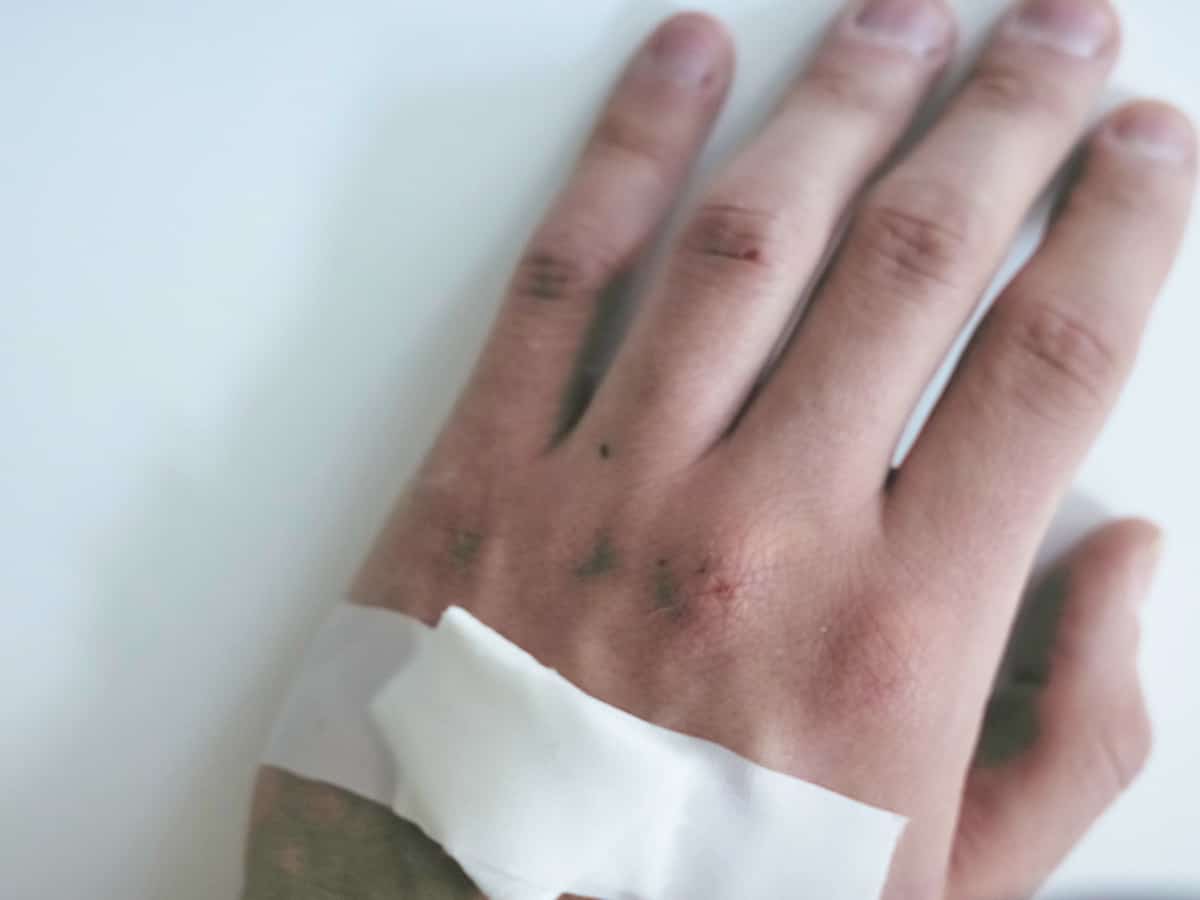
MonkeyPox virus is transmitted from infected animals to humans via indirect or direct contact. Human-to-human transmission can occur through direct contact with infectious skin or lesions, including face-to-face, skin-to-skin, and respiratory droplets, says the WHO.
Typical symptoms include fever, rashes on the body, back pain, headache, swelling of lymph nodes and low energy levels in the first five days. Some experts are equating the symptoms to those seen earlier with smallpox. Incidentally, smallpox was eradicated in the 1980s.
In the current outbreak countries and amongst the reported MonkeyPox cases, transmission appears to be occurring primarily through close physical contact, including sexual. Transmission can also occur from contaminated materials such as linens, bedding, electronics, clothing, that have infectious skin particles.
According to Dr Ishwar Gilada an infectious diseases expert, especially of HIV/AIDS quoted in the media, “MonkeyPox is just like any other sexually transmitted infection. Almost 99% of the cases are homosexual behaviour linked and 80% of them are in Europe followed by Canada, Australia and the US.”
There is no definite treatment for MonkeyPox at present. However, some experts feel that the smallpox vaccine could be useful as a preventive measure and also as a therapeutic agent in treatment. The best and practical approach for now would be to take precautions and avoid any stigma or discrimination of the patients. Will a vaccine needs to be developed like the COVID-19? Only time will tell.
The Indian scenario
Though the number of cases is just a handful in the country at present the worrisome aspect is the detection of cases with no foreign travel record too. The 34-year-old Delhi man admitted into the Lok Nayak Hospital seems to have contracted it within the country as he has no travel record.
In the case of the latest suspect from Kamareddy in Telangana State, the 40-year-old had returned from Kuwait on July 6. He developed fever on July 20 and progressed quickly with other symptoms forcing the doctors to shift him to the Ronald Ross Institute for Tropical and Communicable Diseases in Hyderabad on Sunday,
Similarly, the three cases from Kerala had a history of travel to the Middle East. In view of this initial trend the Union Ministry of Health has called for a look out for patients with unexplained rashes and a travel record in the past 21 days to countries that are experiencing rising cases.
The biggest consolation as of now is that MonkeyPox virus is not lethal. However, countries like Spain, UK, US, Germany are showing that it is highly transmissible. Spain has reported an average rise of over 500 cases a week in the recent past.
The strategy required
In view of this trend, the Director General of Health Services held a high level review meeting in Delhi. Consequently, the National Centre for Disease Control (NCDC) has been asked to undertake an extensive epidemiological investigation of the positive cases so far.
The NCDC has in turn instructed states and Union territories to move suspected cases to an isolation centre and keep them until the entire treatment is completed and the physician gives his nod to discharge. In the event of a continuous increase in cases, the government could start random screening of people arriving from affected countries too.
As far as the WHO was concerned in view of the limited testing capacities in the South East Asian Region, it is coordinating with four laboratories to serve as referrals — National Institute of Virology, India; Victorian Infectious Diseases Reference Laboratory, Australia; National Institute of Health, Department of Medical Sciences, Thailand; and Faculty of Medicine, Chulalongkorn University, Thailand.
Given the nature of its spread the MonkeyPox virus seems to be posing a potential threat akin to an epidemic of HIV/AIDS. India has managed that epidemic with the sustained efforts of public health messaging, awareness on prevention and medical treatment through the network under the National Aids Control Organisation (NACO) with its State units in the last 25 years.
With the fight against the COVID-19 pandemic still continuing, the fresh march of the MonkeyPox virus globally poses fresh challenges to the heavily burdened public health system. But, the experience and lessons learnt from the pandemic should keep us in good condition to face the health emergency in the offing.



